As we discussed last week, understanding the different causes of chronic pain can help to explain the underlying issues and appropriate interventions. Let’s continue with spinal stenosis this week.
Spinal Stenosis:
Spinal Stenosis is a narrowing of the areas in the vertebral body where the spinal cord rests or nerves exit. When narrowing occurs, either the cord or the exiting nerves are compressed because the space to maneuver in is compromised. This causes pain, numbness, weakness in the arms or legs, even bladder and bowel loss, or sexual dysfunction. Compression generally happens more often in the lumbar region, followed by the cervical, and then thoracic spine. This process takes time to evolve, so the symptoms are usually gradual in onset. Diagnosis is based on symptoms and imaging studies.

Think of the back as a series of large round bones that become larger as you descend to the lower back. These are called vertebral bodies. There are seven in the cervical spine, 12 in the thoracic (rib cage area), and five in the lower back and lumbar region as it enters the sacrum and the coccyx (tailbone). Looked at from the top, the vertebral bodies have a hole in the middle, like a doughnut. Coming off the outside of the each doughnut are three bony extensions.
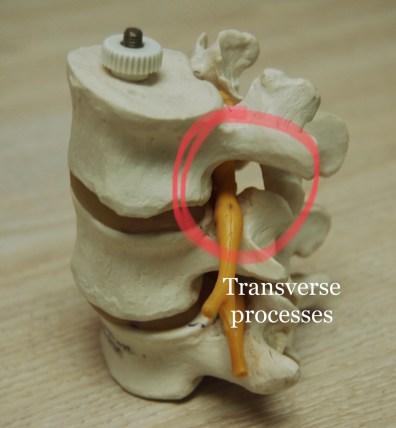
To each side are the transverse processes. These also have holes (the neural foramen) in them and allow the nerves at each spinal level to exit the cord and innervate specific muscle groups into the extremities. The poster bony extension is the spinous process. These are the protrusions you can feel all along your back.

The center hole surrounding the cord (the transverse processes), where the nerves exit, can become smaller as we age due to arthritis that thickens the ligaments, degenerative changes that cause bone spurs, surgery, trauma, endocrine or metabolic abnormalities, and in a fewer cases, congenital disorders.
The resulting narrowing is called stenosis. When this occurs, any motion can create stress on the spinal cord or nerves at that level. That then diminishes the nerve impulses that can get to the muscles. The more you try to use the muscle, as with walking, the less they can function and the more pain you have. Surgical patients are also prone to stenosis because the area has already been impacted and breaks down with time. Degenerative changes increase as we age due to lack of use. That’s another reason why stretching and appropriate daily mobilization is imperative to increase the circulation and keep the ligaments and surrounding areas strong.

Learning the evolution of the condition causing pain, and mechanisms to resolve symptoms can be of value. Some options are:
- bracing
- rest
- ice or heat
- non-impact exercises
- maintaining a heathy body weight and lifestyle
- Tylenol and anti- inflammatories or NSAIDs such as ibuprofen (if no contraindications)
- physical therapy
- injections
- limiting inciting activities
Surgery is usually a last resort when conservative treatment fails.
Unfortunately, after our teen years, very few of us really move the lower lumbar spine. Most of our movement occurs at the junction of the rib cage where it attaches to the lower back. Performing specific exercises where you feel the pull in the tailbone will help prevent it from narrowing and closing down. Talk to your healthcare provider before doing such movements to ensure it’s safe and not harmful to another area or inappropriately stress a previous surgical site.
When the opening for the spinal cord or nerve roots are smaller than normal, any movement can cause inflammation and impingement on the cord and nerves, resulting in back and/or pain in the extremities. A classic complaint is that standing and walking worsen symptoms and rest gives relief. This symptom is called neurological claudication. As you stress the leg muscles, they can’t get the required nerve stimulation to function and they eventually fatigue, becoming painful and forcing you to stop the inciting activity. After a period of rest, the inflammation abates and the nerve impulses can then get to the affected areas, diminishing pain, and allowing you to move again.
I remember after my first few lumbar surgeries I would join my daughter, friends and families to the park, zoo, or shopping. In the beginning, the pain was tolerable. After an hour or two, the pain became more unbearable until it felt like I had hit a wall. A solid, immovable wall. I just didn’t have any more steps in me. I was done. Everyone would look at me like I was crazy.
“You seemed fine just a few minutes ago. ”
“What do you mean you can’t go any further, what suddenly happened?”
“What’s the problem, we’re just walking a little bit further?”
It wasn’t so much that anything suddenly had happened, as much as the accumulation of a series of impacts caused by the days activities on my spine and muscles. They could no longer get the nerve flow they required so they finally just stopped functioning. There was nothing more I could do. Nerve impulses were no longer getting to my muscles. Nothing was going to make them work until I rested and allowed time for recovery. I have to admit, even I thought this was crazy. I mean why could I do it for an hour or two and then suddenly not?
The most embarrassing time was when I was sure I could finish off the day at Disneyland with one last ride on space Mountain. I was with a friend and her kids, along with my daughter. We had been at the park for hours and I didn’t want to be the one to spoil everyone’s fun so I forced myself to “deal with it” and keep going. Well. . .if you don’t listen to your body it has a very strong sense of survival and it will shut down! Denial is only tolerated so long, then reality kicks in.
If any of you have been to Space Mountain, you know that it’s a long, long, long, circuitous climb with lots of people in single file waiting to get to the start of the ride at the top of this mountain. Once in line, there’s only one way out. But for me halfway up was all I could tolerate. My legs could not get enough nerve impulses to my legs for even one more step. It was over. I had to sit down in the middle of the floor, in the middle of the line, until the park security brought me a wheelchair and help me to my car! I was so embarrassed. And I could tell that my friends and family were looking at me like I was crazy, thinking “What the heck happened!? You said you were OK!”.
As a doctor you would think I’d know very well what was going on, understand why I hit a wall. But like many patients, I was in denial. I didn’t want to appear weak. I was sure I could push through the pain or that I could deal with it. I couldn’t except it was a physical manifestation of a process I had no ability to stop. A neurologist friend of mine reminded me what was happening and why I can only function so long before it was over – neurological claudication. That helped me realize I wasn’t crazy; there being a reasonable explanation for the events made a huge difference.
I’d like to say I’ve learned my lesson and that type of issue never happened again. I’d be lying. Human ego, being what it is, I still have trouble honoring my limitations and listening to my body’s needs. Especially when surrounded by people I’m afraid won’t understand.
It’s a daily struggle, but I’m learning, and getting better at setting and sticking to my boundaries. Saying I’ve had enough, letting others go on without me, sitting down and taking care of myself.
This is an important step we all need to learn if we’re going to live a fuller life while dealing with our chronic pain.
 -Dr. Courtney
-Dr. Courtney
Header photo credit: teachmeanatomy.info

